Multi-spectral optoacoustic tomography (MSOT): tracking haemoglobin
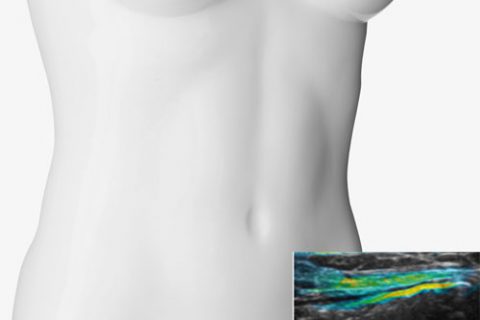
FAU researchers have developed a procedure for locating and measuring quantities of the red blood pigment haemoglobin in intestinal tissue. It is hoped that this will make it easier to check the progress of treatment for chronic diseases, and boost chances of recovery.
Blood supply to tissue increases when organs are inflamed. The organism sends blood cells carrying the red haemoglobin pigment to the site of the inflammation. On the surface of the skin, you can see the inflammation with the naked eye, as the skin takes on a red tinge. Inside the body, however, special instruments are needed to make the body’s activities visible.
A new method for doing so is on the verge of a breakthrough: multi-spectral optoacoustic tomography (MSOT). It allows haemoglobin to be tracked down, and quantities measured. ‘Using this technique we can measure the volume of blood in tissues, giving an accurate indication of the degree of inflammation in bowel disease, for example,’ says Prof. Dr. Maximilian Waldner from the Chair of Internal Medicine I.
MSOT uses the optoacoustic effect which is based on the conversion of light energy to acoustic energy (sound). The principle behind the new technique is that molecules which are excited with lasers in a very high frequency range absorb the energy and reflect it back in a much lower, acoustic frequency range. Based on the frequency spectrum reflected back, accurate conclusions can be made concerning individual molecules and the extent to which they have increased or decreased in the tissue. The MSOT procedure can even be used to differentiate between oxygenated haemoglobin and deoxygenated haemoglobin.
MSOT has a number of benefits compared to other procedures used to examine intestinal tissue. Unlike endoscopies, patients do not need to be sedated or subjected to a surgical procedure. The measurements are completed in a matter of minutes.
Compared to exclusively optical procedures, MSOT offers the advantage of being able to look into human tissue to a depth of up to three centimetres, that is 100 times deeper than is possible using other methods. Compared to normal ultrasound scans, the images are much more detailed. Ultrasound scans only give information about the tissue structure. Using laser, however, individual molecules can be detected.
The optoacoustic effect was described in theory as early as 1880. The problem until now was that the sophisticated technology required to diagnose bowel diseases was not yet available. Now, however, both the required lasers and computing capacities for the digital processing of images are available. ‘Commercial platforms are now available which are suitable for mobile use in hospitals,’ says Waldner. ‘They are just as convenient as traditional ultrasound devices. MSOT is becoming suitable for everyday use.’
Patients suffering from a chronic inflammation of the bowel currently have to wait several months before they can tell if the chosen method of treating conditions such as Crohn’s disease or ulcerative colitis is having an effect. This can lead to delays in finding out which treatment is most likely to be successful and prolong the patient’s suffering.
Initial tests monitoring the patient’s condition using MSOT have raised hopes that the effectiveness of treatment will soon be able to be tested with little effort and at much shorter intervals. The MSOT readings came in nearly all cases to the same conclusion as the subsequent endoscopic examinations. The challenge, according to Waldner, is that ‘up to 50 percent of treatments do not work the first time. ‘It would a be a major step forward if we had a reliable and straightforward method to determine whether the inflammation has already receded.’
by Frank Grünberg
Here we present four further imaging methods:
Endomicroscopy: Rapid test for polyps
Computer tomography: weight-bearing scans
Light-sheet microscopy: an underground train system for immune cells
Endomicroscopy: diagnosing tissue without artificial contrast agents
FAU research magazine friedrich
 This article first appeared in our research magazine friedrich. You can order the print issue (only available in German) free of charge at presse@fau.de.
This article first appeared in our research magazine friedrich. You can order the print issue (only available in German) free of charge at presse@fau.de.